The use of opioids for pain relief in patients waiting for hip and knee replacements increased significantly during the pandemic as patients waited longer for surgery, according to new research.
The University of Aberdeen study found that the numbers of patients using opioids while waiting for surgery increased by 40% compared to pre-pandemic levels.
The surge in opioid use for pre-operative pain was associated with the waiting time for surgery which was an average of 90 days longer during the pandemic as hospitals shifted to focus on providing acute care.
Opioids such as morphine and tramadol are often used as a last resort in pain management in osteoarthritis, however, researchers said there is growing evidence it can be of limited benefit and even long-term detriment to health, especially in older adults.
Long-term opioid use before surgery has also been associated with increased risk of complications related to the operation, poorer outcomes, and ongoing opioid dependence.
Luke Farrow, clinical research fellow at the University of Aberdeen’s Institute of Applied Health Sciences, who led the research, said alternative ways of managing severe arthritis pain must be found “urgently” for those waiting for this kind of surgery.
He said: “Our work provides evidence of potential for an emerging opioid problem associated with the influence of Covid-19 on elective orthopaedic services.
“With continued delays in the provision of timely total hip and knee arthroplasty expected for some time due to the considerable backlog of patients awaiting surgery, patients will need to seek alternative treatment options to manage their symptoms.
“We would advocate that healthcare professionals and patients avoid the use of opioid medication if at all possible due to the known lack of effect in this setting and potential for harm.
“We urgently need to find better alternative methods for managing severe arthritis pain for those awaiting this type of surgery and work to recover the backlog of associated operative cancellations during Covid-19 to prevent to prevent more widespread opioid use.”
The study looked at data collected from 452 NHS patients from the north east of Scotland who were on the waiting list for hip and knee replacement surgery and compared the numbers of patients who had been prescribed opioids with those who had surgery before the pandemic.
The pandemic led to the widespread postponement of elective orthopaedic procedures as hospitals focused on acute care.
Researchers said that patients awaiting hip and knee replacements, as one of the most common elective procedures, have been disproportionally affected.
Estimated figures suggest that more than six million elective orthopaedic procedures were cancelled worldwide during the first peak of the pandemic.
Farrow said: “Whilst these changes have served to flatten the curve and reduce some of the harm associated with Covid-19 infection, there has undoubtedly been an impact on patients whose elective procedures were postponed.
“Covid-19 has had a significant detrimental effect on access to hip and knee surgery, and work by others has suggested this has been associated with worsening pain and quality of life for patients.”
The research is published in the BMJ Quality & Safety.
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


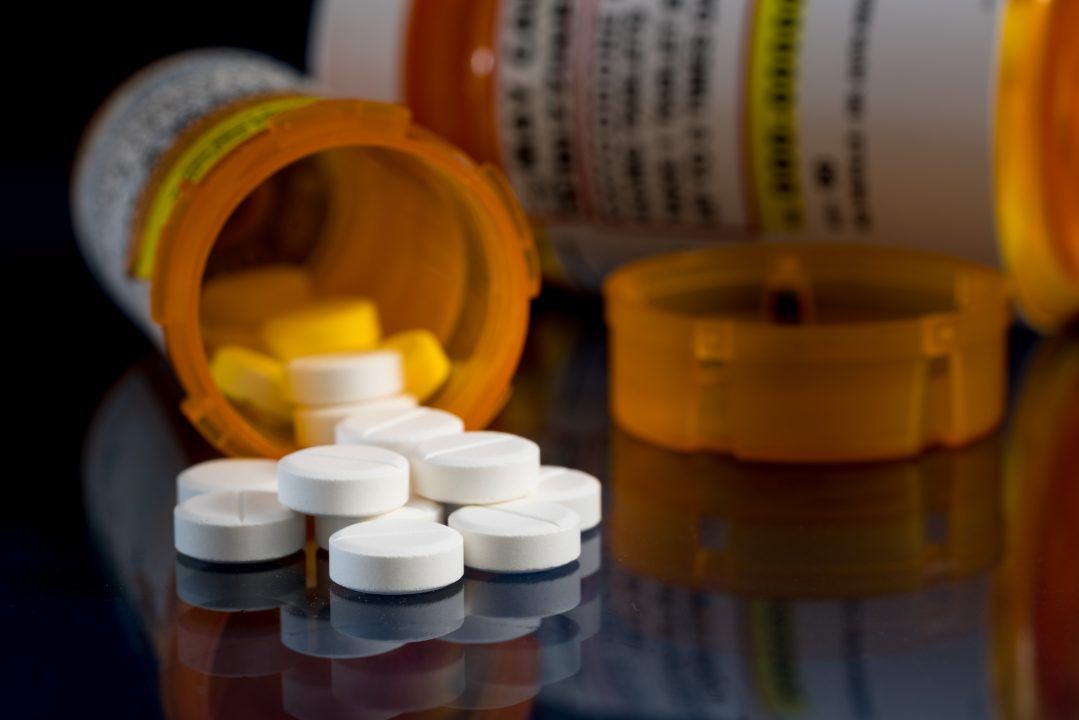 iStock
iStock