The NHS may never be restored to pre-Covid levels of care, a leading doctor has warned.
Dr Andrew Buist, of the British Medical Association (BMA) in Scotland, warned it is going to take “many years” for the health service to recover from the impact of the pandemic – adding he is “not convinced we will ever get back to where we were”.
His said Scotland’s hospitals “cannot hope to function” if the system for providing care in the community fails under the “immense” pressure resulting from the Covid pandemic.
Dr Buist, chair of the BMA Scottish GP committee, added that he fears for the well-being of family doctors, saying the demands they face are “huge and often beyond our capacity”.
He used a speech to the Scottish Local Medical Committee conference – which was attended by health secretary Humza Yousaf – to call for better staffing across primary care, saying “this is something the Scottish Government urgently needs a credible plan to improve on”.
He also urged ministers to embark upon a “genuine, open and honest conversation with the public” about the future of care, saying an expert group should be set up to consider this issue.
Speaking about how the Covid crisis has “greatly disrupted” the NHS, he said: “Waiting times for hospital investigations and treatments have rocketed, the pressures on social care are immense and, in many ways, they are currently the most pressing – because if care in the community fails, then hospitals cannot hope to function.
“That is why I believe it is so important when we think about health care as a society that our focus is not solely – or even primarily – on hospitals.
“It is going to take many years for the NHS to recover from the pandemic. Indeed, I am not convinced we will ever get back to where we were.
He continued: “The pandemic has exposed what many of us knew pre-pandemic – namely that our healthcare model and the way the system operated was unsustainable in the face of rising demand, caused at least in part by an ageing population.
“In world terms we are a wealthy country, but our resources are not unlimited. Pursuit of impossible targets within ever-more stretched budgets raises expectations that cannot be fulfilled, frustrating the public, burning out our workforce and leading in some cases to energies being invested in obstruction, diversion and a culture dominated by fear and blame.”
He told how staff supply within primary care has become a “problem”, adding that the development of new community services has been “significantly held up by a lack of available healthcare workforce”.
Dr Buist demanded: “This is something the Scottish Government urgently needs a credible plan to improve on.
“We need the physiotherapists, the pharmacists, the nurses, who are all key parts of the multi-disciplinary teams we need in place if we are truly to deliver the vision the contract sets out.
“The pandemic has only underlined the importance of all professionals working closely to deliver the right care to patients from the right person – so we need proper strategic planning and a redoubled focus on delivering these staff to support practices across the country, and we need that urgently.”
He also stressed the need to “review what we are trying to achieve through our health care system”.
He urged the Scottish Government to “commit to deliver a genuine, open and honest conversation with the public and key stakeholders to build a realistic achievable vision of what we in Scotland can, and should, provide to our people within the constraints of care, free at the point of delivery”.
This work should be supported by setting up an expert group to “build this vision” of “better care in the community and our hospitals for generations to come”, he said.
His comments came at a time when he said GPs are coming under increased pressure.
Dr Buist said: “GPs are a resilient group, but we are tired. The demands we are facing are huge and often beyond our capacity – I fear for the well-being of individuals trying to do their best and it not being enough.
“The Government and the public must appreciate the GP service or they won’t know what they had until it’s gone – the independent contractor model has served the country well since the beginning of this NHS, but there are limits to which GPs can be exposed.”
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


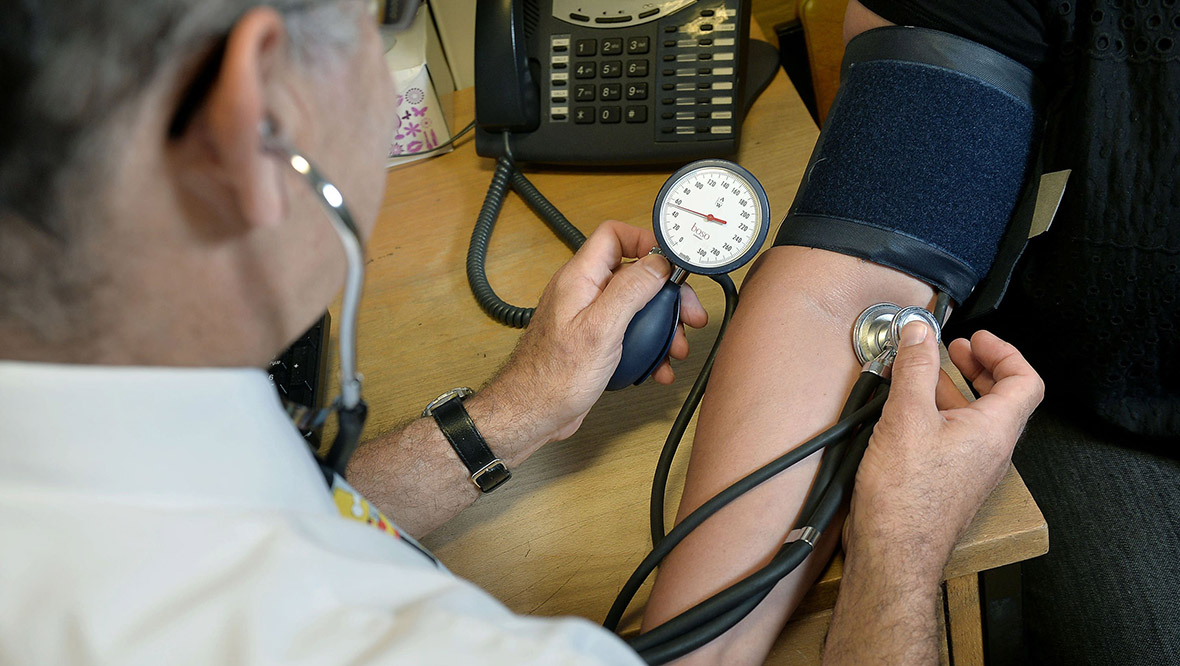 PA Media
PA Media