The number of people with monkeypox in Scotland is continuing to rise, with the latest figures showing a total of 65 cases in the country since late May.
The World Health Organisation last month declared the outbreak – in more than 70 countries – as a “global emergency”.
Following that announcement, large queues have formed at pop-up centres offering smallpox vaccines in London. Further afield, both New York and California have declared public health emergencies in a bid to tackle the outbreak.
STV News takes a look at the latest situation in Scotland.
Who is currently being offered the vaccine in Scotland?
The vaccine is currently being offered to people at higher risk of coming into contact with monkeypox due to limited supplies.
The NHS says more people will be offered a first dose as more supplies become available.
Scotland’s sexual health services have already started contacting people at highest risk to offer vaccination and further eligible groups over the next few months.
This may be done by phone or at your next appointment, for example for PrEP or hepatitis B.
Furthermore, if you’ve had significant contact with someone with monkeypox, you may be offered the vaccine. This includes healthcare workers or through sexual contact.
The vaccine is most effective when given within four days from the date of exposure. However, it can be given up to 14 days after exposure if you’re at high risk of ongoing exposure or at risk of more severe disease.
You can find your nearest sexual health service here.
What is the vaccine?
Monkeypox is caused by a virus similar to the one that causes smallpox. Vaccines designed for smallpox are, therefore, considered effective against monkeypox.
The vaccine used in Scotland contains a virus that’s been modified so that it cannot grow in the human body.
This Modifed Vaccinia Ankara (MVA) vaccine is considered a much safer form of the smallpox vaccine. It’s not specifically licensed for the prevention of monkeypox in Europe, but it’s been used before in the UK against the viral disease.
Imvanex is the brand name for the MVA vaccine, which helps the immune system produce antibodies against the smallpox virus. That means the body’s natural defence system makes its own protection.
MVA vaccines do not contain the smallpox virus and they cannot spread or cause smallpox. The UK Health Security Agency (UKHSA) and the Joint Committee on Vaccination and Immunisation (JCVI) both recommend the MVA vaccine to help prevent monkeypox.
What is the current public health guidance?
The risk of catching monkeypox in Scotland currently remains low.
Guidance from the UKHSA for close contacts of a confirmed monkeypox case has been updated to advise that close contacts do not need to isolate at home for 21 days if they do not have symptoms.
Close contacts are advised to call NHS 111 or a sexual health clinic if they develop a fever or any monkeypox symptoms, and to avoid skin-to-skin contact with others, avoid international travel if possible and to let health or dental facility staff know they are a close contact before attending appointments.
Because it can take up to three weeks for symptoms to appear after being in contact with someone with monkeypox, people are advised to stay alert for symptoms after having skin-to-skin or sexual contact with someone new.
What are the symptoms?
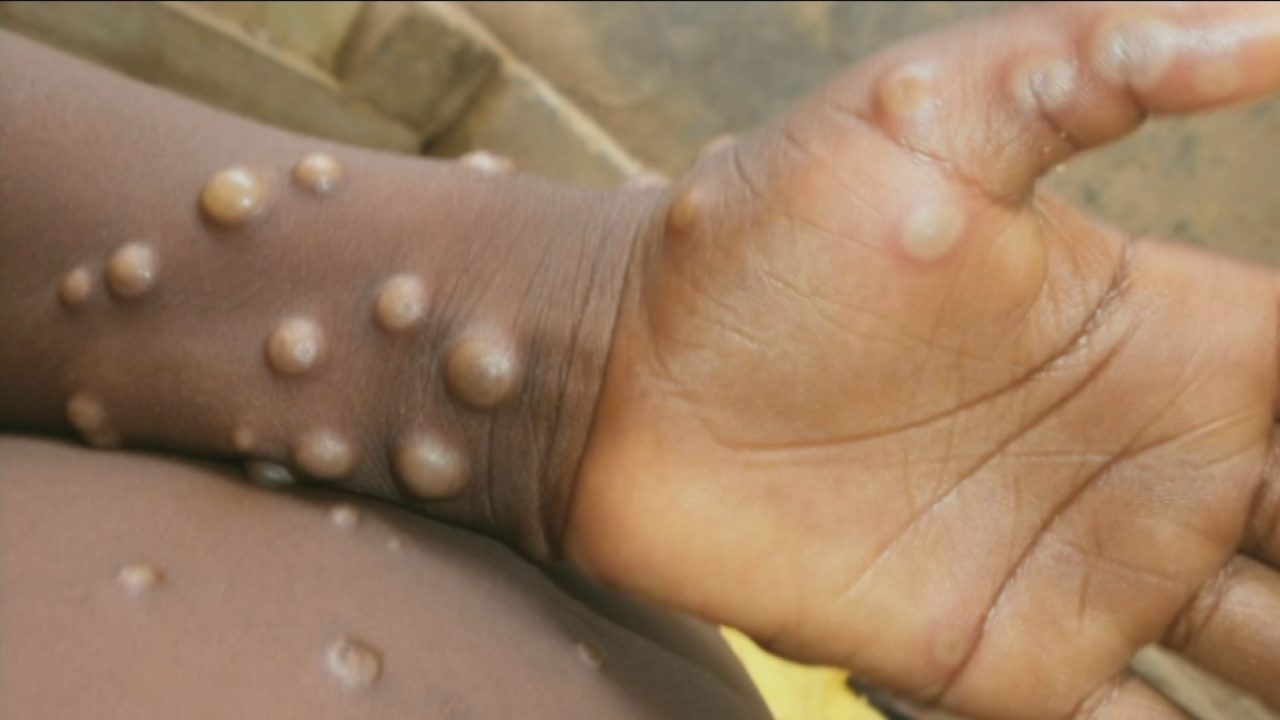
Most monkeypox patients experience only fever, body aches, chills and fatigue, but some may develop a rash and lesions on the face and hands that can spread to other parts of the body.
The rash can look like chickenpox or syphilis, and scabs can form which then fall off. Most people recover within a few weeks.
The incubation period of monkeypox is usually from six to 13 days, but can range from five to 21 days.
How does monkeypox spread?
The most likely route of monkeypox transmission is close physical contact, touching clothing, bedding or towels used by someone with the monkeypox rash, or touching monkeypox skin blisters or scabs.
There is a smaller risk of it being spread through coughs and sneezes, and as prolonged face-to-face contact would be needed, this is not one of the main routes of transmission for the monkeypox virus.
Sexual intercourse is thought to expose people to a higher risk of contracting the disease as, although it is not known to be sexually transmitted, the close physical contact involved means exposure is more likely.
A majority of the cases seen so far have been in gay and bisexual men and men who have sex with men.
How have health agencies in Scotland responded?
Public Health Scotland say monkeypox is generally a mild self-limiting illness, spread by very close contact with someone who is already infected and has symptoms.
Last week the guidance for close contacts was updated and such individuals no longer need to isolate at home if they don’t have symptoms.
Dr Nick Phin, director of public health science and medical director at Public Health Scotland, said: “We continue to ask the public to be aware of the signs and symptoms of monkeypox, particularly as there are a number of large social events happening across the country currently.
“Anyone can get monkeypox and it is passed by close skin-to skin contact with someone who has the infection. Simple measures like checking for unusual blister-like rashes or blister-like sores on any part of the body before attending an event or party can make a real difference.
“By noticing a possible infection early and seeking medical advice, we can prevent onward spread within our communities.”
As of noon on Monday, August, 1 there have been 65 laboratory-confirmed cases of monkeypox reported in Scotland since May 23.
Why has the WHO declared a global emergency?
There are now more than 16,000 reported cases from 75 countries and territories, and five deaths, WHO director-general Tedros Adhanom Ghebreyesus said – up from 3,040 cases in 47 countries around a month ago.
He acknowledged that the committee was unable to reach a consensus on whether the outbreak represents a public health emergency of international concern.
But he said this is an outbreak “that has spread around the world rapidly, through new modes of transmission, about which we understand too little, and which meets the criteria in the International Health Regulations” and he had therefore decided that it should be declared a global emergency.
Previously declared global health emergencies are Covid-19, Ebola, and Zika.
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


 World Health Organisation
World Health Organisation