The number of cases of monkeypox in the UK are expected to increase “substantially”, according to a public health official.
It comes after the first case of the virus in Scotland was recorded on Monday, with the individual who has tested positive being managed in an infectious disease unit.
The individual has not travelled abroad and is likely to have had exposure to it within the UK, it is believed.
So far, there have been 20 cases recorded in England, one in Scotland, and none in Northern Ireland or Wales.
An update was provided by Public Health Scotland on Monday afternoon.
Dr Nick Phin, director of public health science and medical director at Public Health Scotland (PHS) indicated that the number of cases is expected to rise.
For most people who contract the virus, symptoms will include a fever and malaise, before the emergence of flat spots.
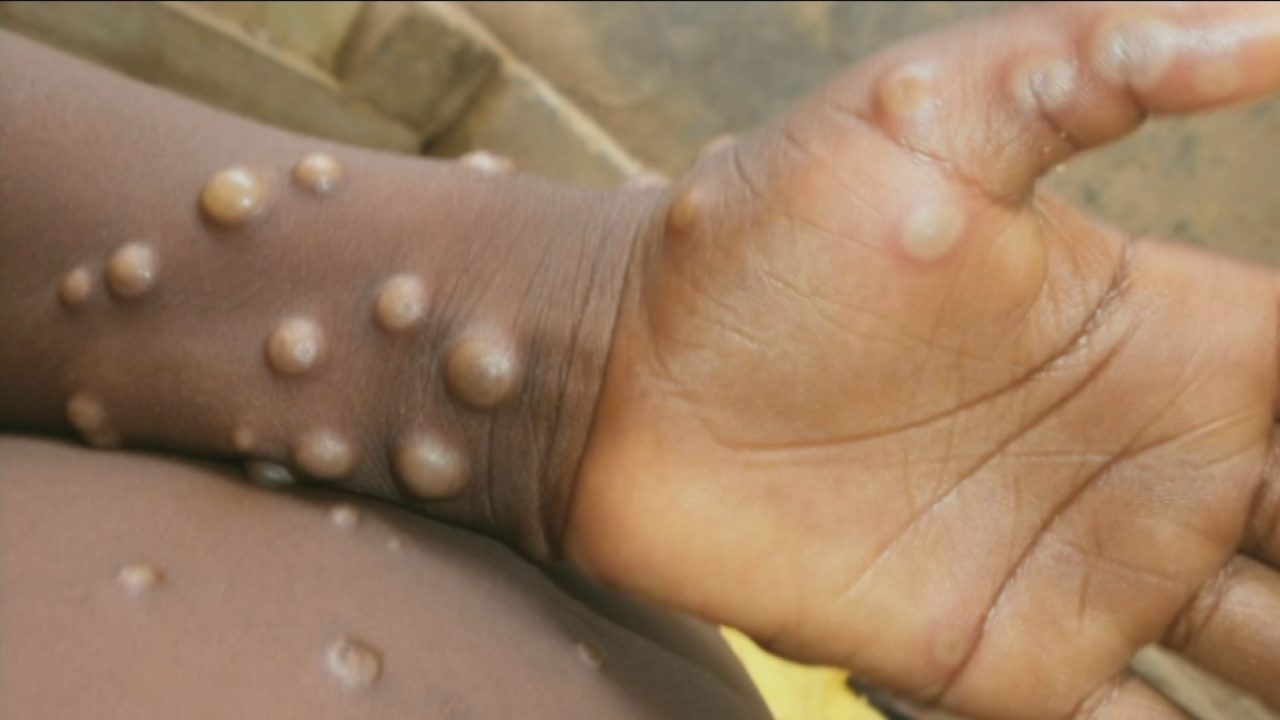
Those spots then over a 24-hour period become raised, before becoming vesicles – similar to serious blisters that are filled with either blood or clear fluid.
The vesicles then become pustules before finally scabbing over and dropping off.
People are considered to be infectious from the point at which symptoms start until the scabs fall off and there is fresh skin there, which can take around three to four weeks.
Dr Phin explained that the vesicles are the most infectious, as the dried scabs can contain large amounts of viral particles and can infect others.
There is a vaccine available for the virus, called Imnavex, which is licenced in the US for the management of monkeypox.
In the EU, the vaccine is only licenced for use on smallpox, but the licence is expected to be extended for the use of managing monkeypox as well.
There is a supply of vaccines in Scotland, with drug treatment supplies being ordered in, in liaison with the UK.
Dr Phin ruled out the suggestion that the virus is “Covid 2” and explained there are “striking differences” between the viruses.
Those include having an effective vaccine for monkeypox, no asymptomatic phase of the virus, and is easier to identify.
“I’ve no doubt that when the UKHSA (UK Health Security Agency) update the figures today, you will see that will have increased and reasonably substantially,” he told a briefing on Monday.
“The infection itself, it’s not common, it’s associated with close contact and the close contact can either be through broken skin, through mucus membranes or through inhalation of droplets.
“Or sometimes the sort of dander, the skin that you can get accumulating on surfaces, so we call them fomites.”
Dr Phin outlined that the key issue around transmission of the virus is through close contact.
He said: “It’s close contact that’s the key issue and once someone is exposed, the incubation period, depending on which group you read, it’s either between five and 14, seven and 21.
“But we’re in that broad range of about a week to three weeks, with most appearing in the first two weeks.”
The public health official explained that those who are immunosuppressed could experience a more serious condition.
“The people that are most susceptible and obviously could get potentially more serious illness are people that are immunosuppressed, people like pregnant women,” he said.
“So that sort of particular group where immunosuppression may be a feature either of their treatment, the diseases, or their conditons.
“And in those people you can see a more serious condition.”
Dr Phin set out the chances of transmission in a crowded place, if someone had symptoms.
“If you were living on your own, you didn’t see anyone, then fine, it wouldn’t spread,” he said.
“But if you were part of a crowd, and let’s say you had these vesicles on your hand or your arms, or your face, and no one noticed and you were brushing up against them, then there’s a fairly strong likelihood that it’s possible that transmission would occur.
“So it’s more to do with close nature of transmission, and that really depends on the situation in which the cases present.”
Where did monkeypox come from?
The virus was first identified in 1958 in the Congo, in Central Africa.
It was identified in a group of monkeys who were part of some small pox work.
The virus was first identified in humans in the 1970s.
In Central and Western Africa, rodents and small mammals are the source of transmission.
There was a monkeypox outbreak in the US back in 2003, which investigators determined was caused by a shipment of animals from Ghana to Texas.
The variant that has been identified in the UK is from West Africa, a milder form of the disease.
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


 World Health Organisation
World Health Organisation
























