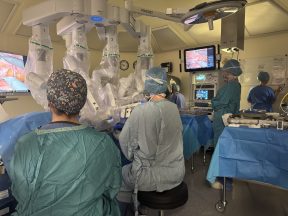
Scotland’s junior doctor workforce is “balancing on a knife-edge”, the chair of the British Medical Association’s (BMA) Scottish Junior Doctor Committee (SJDC) has warned.
Dr Lailah Peel says junior doctors are “exhausted, depleted, and struggling to see the light at the end of the tunnel” due to workload pressures.
Her comments come as the publication of the Scottish Government’s working group report on the 48-hour maximum working week approaches its one-year anniversary.
It highlighted 14 urgent recommendations to be made in order to improve the working lives of junior doctors, however the BMA say that there has been “very little progress” made since as only one – a limit on the number of consecutive long shifts, which are ten hours, to a maximum of four in any seven days – has been implemented.
Other guidance, such as improving rest and sleeping facilities, ensuring a minimum of half an hour of rest after approximately four hours of duty and the provision of basic education on sleep, fatigue and working nights, are all yet to be applied.
Dr Peel said: “Make no mistake, junior doctors in Scotland are angry.
“We are balancing on a knife-edge right now. Morale is rock-bottom, we are exhausted, depleted, and struggling to see the light at the end of the tunnel.
“The workforce is buckling under the current workload pressures and I’m increasingly having conversations with colleagues about their concerns over unsafe working environments.
“Add in this year’s real-terms pay cut and you are looking at a workforce that feels extremely under-valued and I have serious concerns for the wellbeing of my colleagues.”
She added: “Limiting the number of long shifts in any seven days was a key priority for us in our own wellbeing report, and it has of course been reassuring to hear of positive rota changes across Scotland from August.
“However I am still hearing from colleagues who are working rotas which contain five consecutive long shifts, and that’s simply not good enough almost a year down the line from the expert working group report being published.
“It’s also worth pointing out that the report sat gathering dust for nearly two years before it was finally published, so things have been going on much longer than is acceptable.”
She said the possibility of industrial action has been raised, with feedback to a recent pay survey showing it is “clear” that junior doctors are “more prepared for potential sustained strike action than our more senior colleagues”.
But Dr Peel added: “No-one wants to strike. We care deeply for our patients, who are already being impacted by the current situation – and this isn’t a decision we would take lightly, but if things do not improve, I struggle to see how it could be avoided.”
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


 iStock
iStock