A mum diagnosed with cervical cancer in her 20s, despite having no symptoms, is urging women to get checked.
It’s a test many women put off – but one that could make all the difference. Cervical screening can detect early changes before cancer develops, yet uptake in Scotland has fallen.
Vikki Ridler was building her career as an estate agent when a routine smear test shortly after the birth of her second child revealed abnormal cells.
At 23, she began regular monitoring every six months, which continued for four years before she needed treatment.
“I never thought anything of it,” she told Scotland Tonight.
“It wasn’t painful, it wasn’t anything. I just sat and watched that happen,” she added. “The consultant at the time said, ‘Listen, Vikki, I think we’ve got everything. You’ve seen it. We’ll get the results of the biopsy and that might be it.'”
Two weeks later, she received a call she didn’t expect.
“It was very straightforward and very direct – ‘we’ve got the results of your biopsy. The consultant wants to discuss with you. Please come in tomorrow. Please make sure you bring somebody with you.’ As soon as they said that, I knew.”
‘Everyone thinks it won’t happen to them’
 STV News
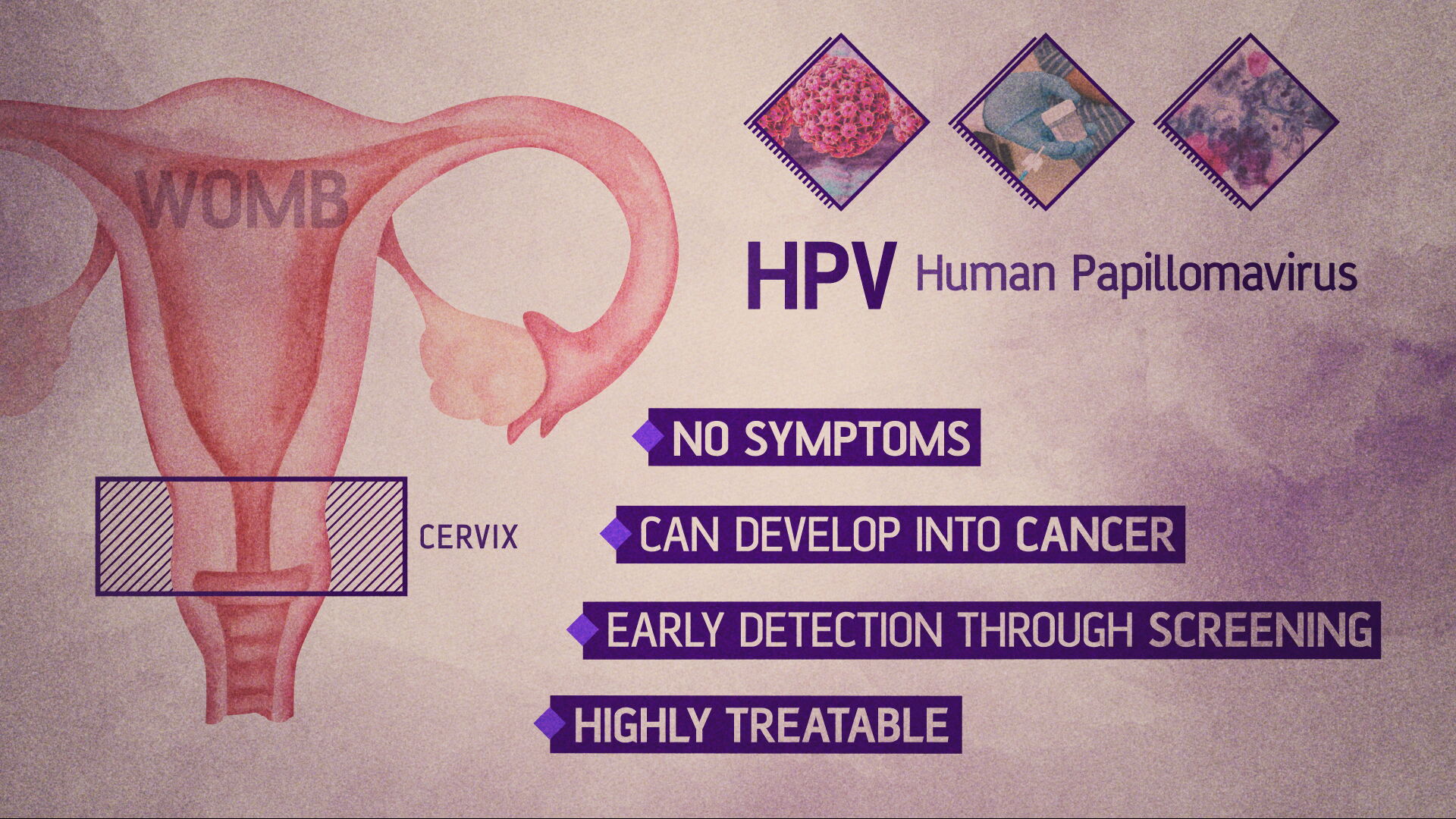
STV NewsCervical cancer affects the cervix – the entrance to the womb. Most cases are linked to a common virus called HPV. It usually causes no symptoms, but can lead to cancer developing over time.
Screening, or smear tests, can spot early cell changes before they turn cancerous, and when found early, it’s highly treatable.
But for Vikki, a biopsy revealed cancer in her cervix.
“Everybody thinks it’s not going to happen to them, but really, cancer does not discriminate at all,” she told Scotland Tonight.
Vikki was facing the prospect of a hysterectomy and endured an agonising four-week wait for an MRI to determine what treatment she would need.
“Everything felt enormous at that moment in time,” she added. “There’s no answer, and it’s probably one of the periods that was the most difficult.”
At just 27, she was trying to come to terms with life-changing surgery.
“The plan was a hysterectomy,” she explained. “It was mentioned to me right at the very beginning.
“I did say at the time: ‘Is there anything else apart from that?’ Because at 27, hearing that, a hysterectomy felt like something an older woman would have.”
‘I was in a dark place after surgery’
 STV News
STV NewsVikki underwent a seven-hour operation, which was a success, and she felt fortunate she did not need further treatment.
“Two weeks later, I went in to get my catheter out and get the news, and it was great because no further treatment was needed,” she said. “I could just focus on getting better and recovering. But recovery was tough.
“I really broke. There’s really no other explanation for it. Who I am and what I am, I sort of lost,” she said. “I just felt completely alone and in quite a dark place. It wasn’t until really understanding how bad I’d got that I was diagnosed with PTSD.”
With help from a counsellor, she began to make sense of what she’d been through.
“There have been so many different changes in my life and for me as a person. My mindset completely changed,” she said. “Something like that makes you appreciate the life that you’ve got.”
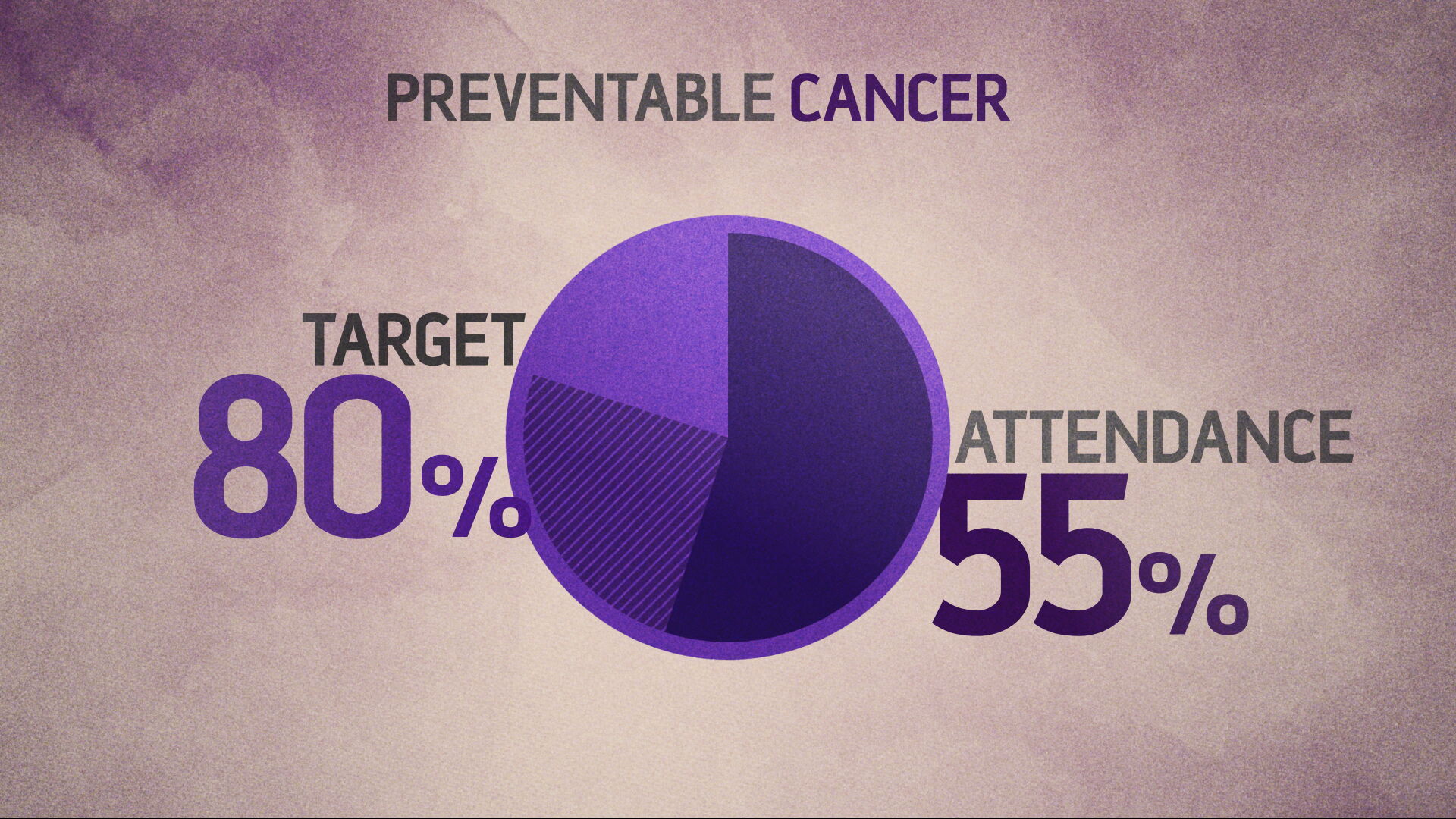
Cervical cancer is one of the most preventable cancers, but just 55% of women attend their smear test. The target set by Public Health Scotland is 80% participation.
‘Numbers have fallen – that concerns us’
 STV News
STV NewsDr Tasmin Sommerfield, director of medical screening for Scotland, said falling screening numbers were a concern.
“Yes, the numbers have fallen. That’s been seen across the whole of the UK and other parts of the world as well, so that does concern us,” she said.
“We really want to get these figures up. We know that the rates have fallen most in younger women and also women from more deprived areas.”
Scotland plans to eliminate cervical cancer by 2040, but that relies on both vaccination and screening.
“Even if someone’s had the vaccination, they should still come for cervical screening,” Dr Sommerfield said. “Cervical cancer can be caused by different types of HPV, and the vaccine covers the main types that cause cancer, but not all of them.
“We want people to be vaccinated, we want them to come for cervical screening when they’re invited, but we’re also really aware of symptoms in between screens, and if they’ve got any concerns to get them checked out by a doctor.”
 STV News
STV NewsThere is also a pilot scheme for women to test themselves for HPV, targeting those who haven’t been participating in cervical screening.
Dr Sommerfield said the self-sampling kit includes a swab and a tube of liquid, similar to a cotton bud.
“We’re very hopeful that it will help engage more women in cervical screening,” she said. “There’s good evidence from other countries that use self-sampling that it does help to improve uptake.
“The standard cervical screening test is still the best test to have, but this is a useful extra step for women who find it harder to engage in screening.”
High-profile cases and women sharing their experience can also have an impact.
 Getty Images
Getty ImagesReality TV star Jade Goody was diagnosed with cervical cancer in 2008 and died a year later at the age of 27. Her story prompted more women to come forward for screening.
Dr Sommerfield said stories like Vikki’s can have a powerful effect.
“We’re tremendously grateful to people like Vikki who share their stories because that makes such a difference,” she said.
Vikki said she is passionate about sharing her experience to help others.
“Please book that appointment. Please go,” she said. “That couple of minutes of not feeling comfortable will give you peace of mind.
“If you’re receiving those letters, or you’re in your mid-20s or anything along those lines, you are in the best possible place for help. There’s always somebody there that can help you – but please, do not ignore it.”
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country






























