Rheumatoid arthritis (RA) patients prone to feeling weak could see their symptoms reversed following treatment, according to new research.
The debilitating condition can affect anyone of any age, and for some can take months, sometimes years, to get an accurate diagnosis, according to Versus Arthritis, the UK’s largest charity dedicated to supporting people with arthritis.
A new study, led by the University of Glasgow, found that frailty is common in people with RA, including in many younger people aged below 65, and people who have it severely are more likely to be admitted to hospital or die.
Researchers have said as people’s RA was treated and became less active, their degree of frailty was also reduced.
They also said early control of the condition can improve symptoms.
Dr Peter Hanlon, clinical research fellow at Glasgow University’s Institute of Health and Wellbeing, said the study, published on Wednesday, is “incredibly encouraging”.
He said while it can be a challenge to identify people for whom reversing frailty is possible, the new research “is incredibly beneficial for clinicians when assessing people with RA and deciding on a broad approach to treatments”.
Dr Hanlon added: “It also suggests care should be taken in applying a ‘label’ of frailty to people living with RA, given the potential to reverse this following treatment.”
The study looked at people with RA identified from the Scottish Early Rheumatoid Arthritis (SERA) cohort – those who are newly diagnosed with an average age of 58 years – and UK Biobank – patients with established RA at an average age of 59 years.
Data showed frailty was common in both the SERA group (12% moderate, 0.2% severe) and the UK Biobank cohort (20% moderate, 3% severe).
Neha Issar-Brown, director of research at Versus Arthritis, said: “This research provides further clear evidence of the importance and very real benefit in people quickly finding the most effective treatment that will reduce the impact of RA and prevent it getting worse.”
The study is published in rheumatology journal RMD Open.
It was funded by the Medical Research Council (MRC) and Versus Arthritis.
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


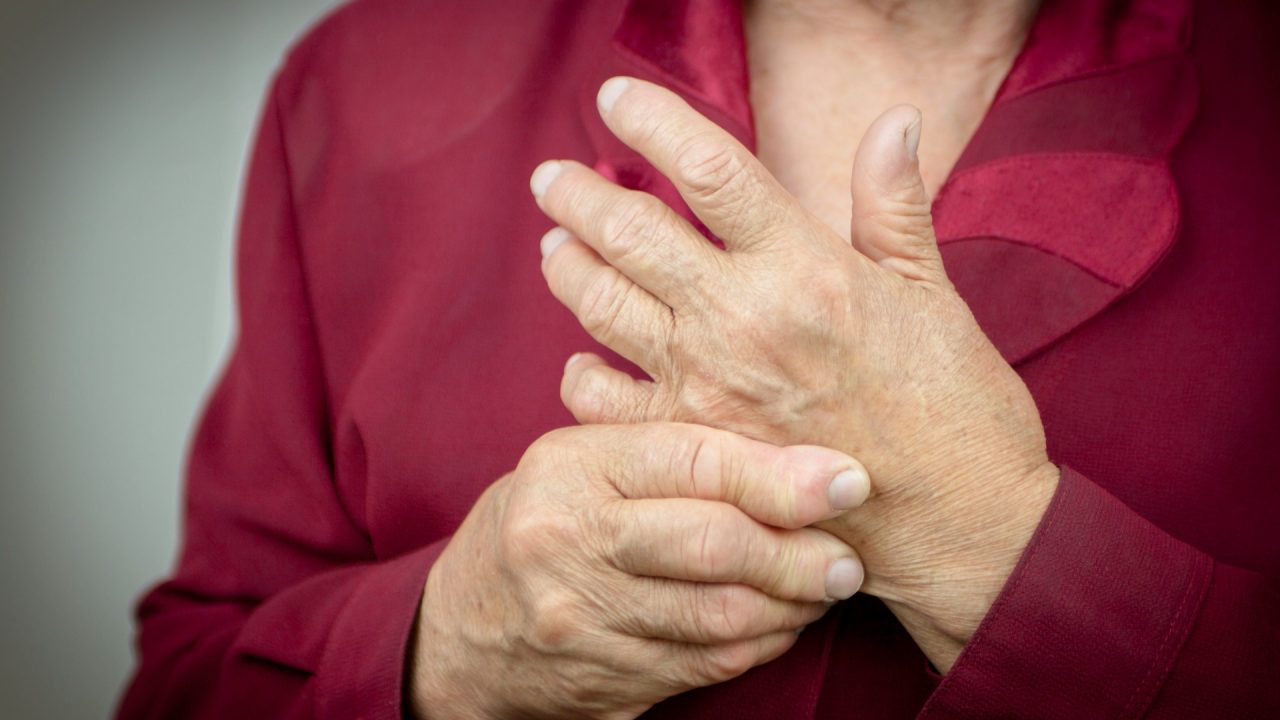 iStock
iStock