Youngsters with eating disorders were left traumatised after being restrained by “heavy-handed” medics and fed by nasal tube – with patients telling inspectors of stressed staff and missed feeds.
Bosses at the Royal Hospital for Children and Young People’s Melville Unit in Edinburgh have been told to improve nine areas of care after inspectors from the Mental Welfare Commission discovered a series of issues at the facility.
Medical staff at the in-patient unit told report authors they were worried they would “lose their nursing registration due to deficits in care” and that it was “physically impossible” to do all required tasks.
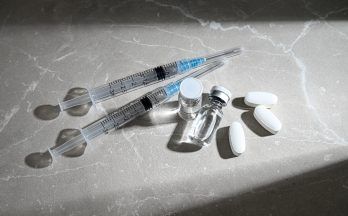
The youngsters, many of whom have eating disorders, told inspectors the unit was “short staffed and is regularly staffed with bank and agency” nurses, and many of these did not have the required training to carry out some tasks in their treatment plans, specifically nasogastric (NG) feeding.
The 12-page report said: “As a result, there have been times when these treatments have not been carried out.
“The young people told us when the unit is short staffed, it causes staff on the shift to be ‘stressed’.
“We were told that some of the young people have felt ‘traumatised’ after NG feeds, due to being physically restrained and staff adopting a ‘heavy-handed’ approach at times.”
“We were also told by some of the young people they had missed NG feeds due to staff shortages and felt angry about the inconsistent message being given to them by staff.
“The young people added that they are told by staff that they ‘must have’ certain amounts of NG feeds in a day, however when the unit is short staffed the NG feeds are not given.
“We heard that at least one of the young people had experienced a deterioration in their physical health following missed feeds.”
Inspectors visited the unit in April and had not planned to return until 2023.
But in August the commission said it received information from staff highlighting “significant concerns in relation to the young people’s care and treatment at the unit, specifically incidents of missed nutrition”.
They went to the 12-bed unit, run for 12 to 17-year-olds with mental health problems, on August 29.
Not all patients had eating disorders and the youngsters who did not “tended to spend long periods of time in their room, which raised concern over increased isolation”, the report said.
All of the youngsters inspectors spoke to said “meal times in the unit were unpleasant”, that there was no choice of meals, and at times they had to eat food they did not like.
“Many of the young people require ‘meal support’ from staff and we were told that there were occasions when staff did not display positive modelling behaviour, for example, making comments about their own eating habits,” the report said.
“The young people did not find this supportive and at times it was ‘triggering’.”
Inspectors also found one patient who felt they did not have control over decisions being made about their care, patients with eating disorders having more comprehensive records than those with a different mental health diagnosis, and a lack of opportunity for nursing staff to have regular therapeutic interventions with the young people.
Staffing was also raised among the concerns of inspectors, with retention and sickness issues seeing agency staff called in, especially at weekends.
“All staff we spoke to told us that they find the current staffing situation in the unit extremely difficult,” the report said.
“Some of the staff told us that it was ‘physically impossible’ for them to complete all tasks recorded on the care and treatment plans of the young people.
“Some staff told us that they do not feel the ward is always a safe working environment for them to work and they are concerned that they will ‘lose their nursing registration’ due to deficits in care.”
They said some senior managers set “unachievable treatment goals” and had “unrealistic expectations” of the care able to be offered at the unit.
“Some of the staff we spoke to told us that they were actively seeking alternative employment,” the report added.
Tracey Mckigen, service director for the Royal Edinburgh Hospital and associated services, NHS Lothian, said: “We remain committed to delivering safe, holistic and person-centred care for all our patients, and actively welcome the visit by the Mental Welfare Commission for Scotland as well as the publication of their report.
“It is encouraging to see improvements noted within the report, however we recognise that more work needs to be done. Immediately following the visit, a robust and detailed action plan was developed, to deliver on each of the recommendations and significant work has already been completed, with further additional work under way.
“We continue to work closely with staff, providing ongoing support and have clear processes in place to ensure safe staffing levels.”
Follow STV News on WhatsApp
Scan the QR code on your mobile device for all the latest news from around the country


 Google Maps
Google Maps